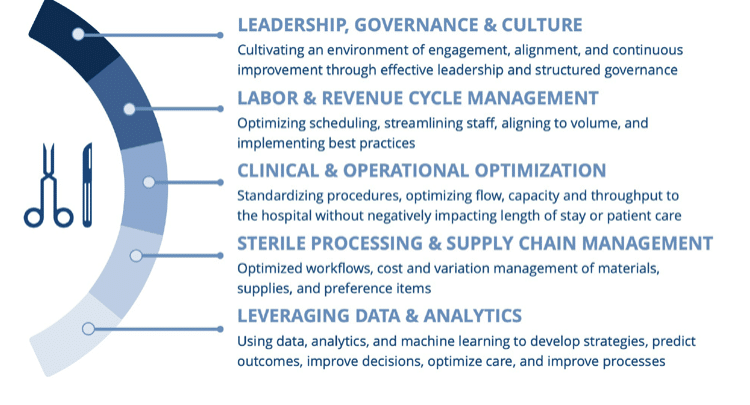
Perioperative services typically account for 50-75% of hospital revenue and 30-40% of expenses. However, many healthcare delivery organizations continue to struggle with perioperative optimization. Success hinges on a collaborative governance structure, taking a holistic approach to optimization, and, perhaps most importantly, working with a partner who has extensive perioperative experience and deep expertise in every aspect of healthcare delivery.
Perioperative Services Can Financially “Make or Break” Your Hospital
Perioperative services are unique. Typically accounting for 50-75% of hospital revenue, and 30-40% of expenses, perioperative services is one of the only departments that can single-handedly “make or break” a health system financially. Despite the high clinical and financial stakes, many healthcare delivery organizations continue to struggle with implementing standardized perioperative procedures and best practices, such as those related to scheduling, preauthorization, block time management, turnover, preference cards, and supply pulls. Additionally, there is often a lack of leadership and perioperative governance necessary to effectively drive continuous performance improvement and staff engagement.

Keys to Successful Perioperative Optimization
Optimizing perioperative services represents a significant opportunity to improve your patient outcomes, hospital margins, and surgeon satisfaction. However, capitalizing on that opportunity requires that your organization:
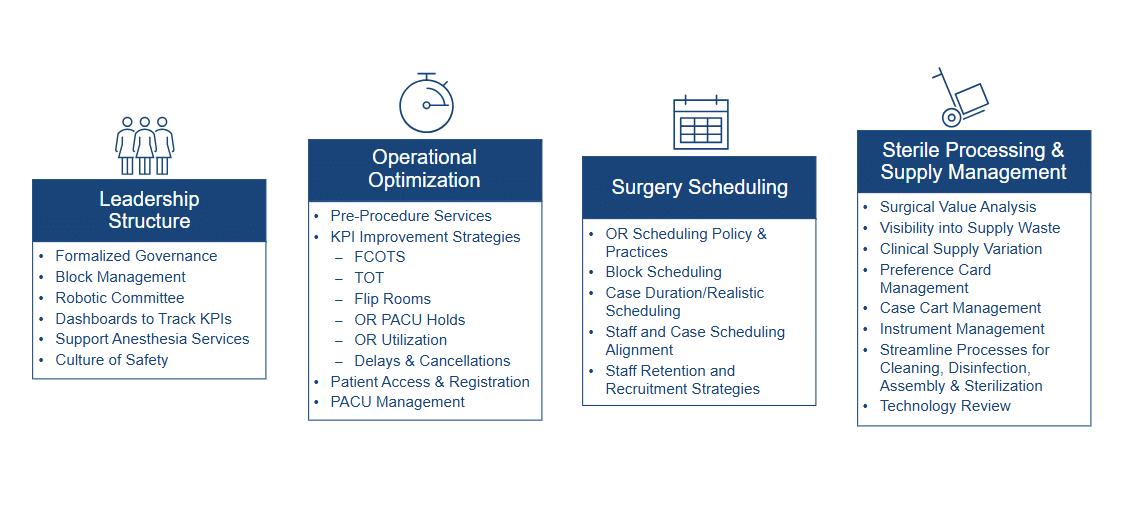
- Ensure that a collaborative perioperative governance structure is in place. Successful perioperative optimization begins with a formalized and collaborative governance structure that has clear goals and a well-defined charter that serves as the “guiding light” for decisions that support the organizational strategic goals. Participation needs to include stakeholders from nursing, surgery, and anesthesia; true perioperative optimization is impossible without input from all three. The designated nursing, surgeon, and anesthesia leaders need to work closely on a regular basis to not only develop standardized best practices but also foster a culture of safety that ensures the best possible outcomes for patients. There are a myriad of things that can go wrong in the operating room. Staff at any level – and at every point in the patient’s journey – need to feel empowered to speak up when they see something that could result in patient harm or a poor outcome. The perioperative governance structure must be fully aligned with your hospital’s strategic plan. For example, block utilization is crucial for surgeons. Well-defined block utilization guidelines and standards for allocation qualification, review, and adjustment are essential, but those guidelines and standards ultimately still need to reflect your organization’s unique strategic priorities.
- Take a holistic approach to perioperative optimization. Optimization of perioperative services starts in the clinic as soon as the decision is made that a patient requires surgery – and it continues until the patient is discharged from the hospital or transitioned to the next level of care. The scope of factors that need to be carefully considered to fully optimize perioperative services is massive. Opportunities for improvement in both care and efficiency exist at several points in the patient journey, from scheduling to discharge, and the impacts are felt across multiple functions, including the revenue cycle and supply chain. There can be a tendency for some hospitals and health systems to narrowly focus only on “high profile” perioperative metrics related to block time or turnover time. While those KPIs are highly valuable, it is important to remember that numerous factors contribute to any failures the measures reflect – many of which need to be addressed well before the patient arrives for surgery. For example, the patient may not have been prepped appropriately or may not have received the right pre–admission testing. Maybe it wasn’t clear what surgery was scheduled, and the wrong preference card was pulled. The reality is there are countless considerations related to optimization that need to be carefully examined throughout the patient’s journey, not just during their time in the OR. Understanding the underlying reasons driving fluctuation in core perioperative metrics is the only way to effectively act on them.
- Work with the right consulting partner. Optimizing perioperative services represents an extremely valuable opportunity for any hospital, but success requires navigating a highly complex environment with many interdependent processes. Given that many health systems may lack the necessary bandwidth, resources, or expertise, finding the right partner is crucial. Any partner should have staff with years of firsthand clinical and operational experience in perioperative services as well as proven results successfully navigating improvement. The right partner should know common perioperative pain points – and best practices – across the patient’s entire journey. Operational and clinical excellence needs to be the priority. The sheer scope of hospital functions that impact perioperative services – and that perioperative services impact – means the right consulting partner also needs extensive knowledge of every aspect of healthcare delivery, ranging from patient flow and throughput, EHR optimization and integration, supply chain, revenue cycle, and physician services. A true partner needs to work collaboratively with health system leadership to identify opportunities and drive value predicated on quality patient care and efficient throughput.
The Bottom Line
Optimized perioperative services improve patient outcomes, hospital margins, and surgeon satisfaction. Success hinges on establishing a collaborative governance structure, taking a holistic approach to improvements, and working with the right partner.
About Impact Advisors Perioperative Optimization Services
Led by a team of former perioperative clinicians and supplemented by operations and technical subject matter experts, Impact Advisors uses a systematic and holistic approach to optimize the OR and all procedural areas (e.g., Endo, Cath Lab, EP Lab, and Interventional Radiology). We share valuable insights on common issues and help your team dig into your organization’s unique challenges to find solutions.